Key Facts
- Zygomatic dental implants are extra-long fixtures (35–55 mm) anchored in the cheekbone, used when severe upper jaw bone loss prevents conventional implants.
- They offer a graftless solution, often avoiding sinus lifts and bone grafts, with immediate loading possible so patients can leave with fixed teeth the same day.
- Success rates exceed 95%, with survival rates around 96–98% over 12–15 years when placed by experienced specialists and maintained with proper hygiene.
- Ideal candidates include long-term denture wearers, failed graft or implant cases, and patients with maxillary defects; costs vary widely by region, ranging from $15,000–$50,000 for a full arch in the U.S.
Severe bone loss in the upper jaw doesn’t have to rule out fixed teeth. Zygomatic dental implants anchor in the cheekbone, bypassing weak maxillary bone and often avoiding sinus lifts or large grafts. Lengths of 35–55 mm give solid primary stability, which means many patients leave with a fixed provisional bridge the same day. Ideal candidates include long-term denture wearers, failed graft or implant cases, and post-resection defects. If speed, predictability, and function matter, this graftless approach can put full-arch teeth. Continue reading to know more about the Zygomatic Dental Implants.
What Are Zygomatic Dental Implants?
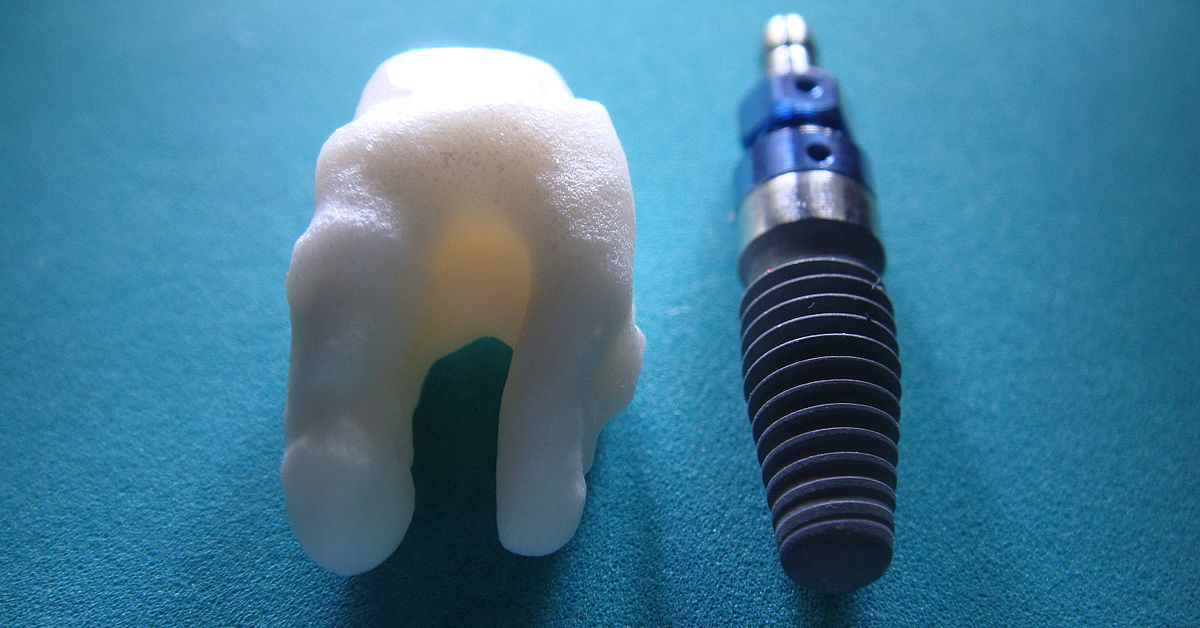
Zygomatic implants are extra-long fixtures that anchor in the cheekbone. Lengths typically range from 35 to 55 millimeters. They bypass deficient maxillary bone to support a full-arch bridge when conventional implants cannot.
Two to four implants are common. Many cases pair them with anterior conventional fixtures for cross-arch stability. In severe atrophy, a quad zygoma provides full support.
Indications and Patient Selection
Use zygomatic implants for patients with advanced posterior maxillary loss. Causes include periodontitis, long-term denture wear, failed implants, trauma, oncologic resection, and congenital deficiency. Select this path when grafting is not feasible, not desired, or time is critical.
Assess expectations and hygiene capacity. Confirm that the patient understands the graftless nature, benefits, and specific risks. Document systemic factors and smoking status.
Advantages Compared With Bone Grafting
This is a graftless solution for severe maxillary atrophy. You avoid sinus lifts and large block grafts, which cuts stages and total time. Immediate loading is common, so the patient leaves with a fixed provisional.
The zygoma is dense and well buttressed. Primary stability is high, which supports same-day teeth in suitable cases. Fewer surgeries and faster function often improve acceptance and overall cost-effectiveness.
Preoperative Assessment and Planning
Start with a full clinical exam, photos, and CBCT. Plan the prosthetic end point first, then place hardware to serve it. Establish vertical dimension, lip support, and smile line before committing to trajectories.
Digital planning and guided surgery help, but judgment still matters. Evaluate sinus anatomy, orbital floor, and zygomatic buttress thickness. Discuss diet, hygiene, and follow-up so the patient knows the playbook.
Anesthesia Options
Most teams choose IV sedation or general anesthesia for comfort. Experienced surgeons can place zygomatic implants under local anesthesia with premedication. Local anesthesia lowers systemic risk and avoids intubation sequelae.
Intraoperative CBCT under local anesthesia can confirm position in complex anatomy. Manage patient anxiety with oral anxiolytics as indicated. Choose the pathway that fits the patient, the surgeon, and the case difficulty.
Surgical Technique
Use extramaxillary or extrasinus paths when anatomy allows to limit sinus contact. Prepare the site at the planned angulation and engage the zygomatic bone with controlled insertion. Target insertion torque between 35 and 45 Ncm.
Protect soft tissues, especially at the emergence profile. Verify multiunit abutment positions for a cleansable prosthesis. Close with tension-free suturing and document primary stability.
Immediate Loading and Prosthetic Sequence
Most suitable cases receive a fixed provisional the same day. The provisional distributes load across the arch and protects the surgical sites. Keep the diet soft during early healing and monitor bite forces.
After soft-tissue maturation and occlusal stabilization, fabricate the definitive bridge. Options include titanium frameworks with acrylic or composite, and monolithic or layered zirconia. Choose materials based on parafunction risk, phonetics, and maintenance strategy.
Risks and Complications
Sinusitis is the headline risk, reported near 14.2 percent in the literature. Extrasinus trajectories and careful planning reduce that risk. Osseointegration failure is uncommon but possible and requires early detection.
Peri-implantitis follows poor hygiene and missed reviews. Train patients on cleaning tools that actually reach under the bridge. Over-torque can damage bone or hardware, so respect the numbers.
Clinical Success and Survival Rates
Published success rates are consistently above 95 percent. Cumulative survival often ranges from 96 to 98 percent over 12 to 15 years. Results depend on case selection, surgeon experience, and prosthetic discipline.
The Zygoma Success Code provides criteria to score outcomes consistently. Track soft-tissue health, sinus status, prosthetic integrity, and patient-reported function. Measure, improve, repeat.
Cost and Economic Considerations
Fees vary by region and scope. In the United States, a full arch often falls between 15,000 and 50,000 dollars. In the United Kingdom, plans commonly start near 10,000 pounds. Markets such as Turkey may charge 1,500 to 5,000 dollars per implant.
Total cost reflects the number of zygomatic and conventional fixtures, anesthesia, provisional and definitive prostheses, and surgeon experience. Graftless treatment often wins on total time and total spend because it removes staged grafting and long delays. Provide an itemized plan so patients see where the value sits.
Longevity: Implants Versus Prosthetic Teeth
The implants are designed to last decades with proper care. The prosthetic teeth will wear and eventually need replacement. Plan for maintenance from day one.
Retrievable designs make service simple. In many cases, you can change a worn prosthesis on the same titanium bar in a single visit. Patients appreciate predictable upkeep more than surprises.
Maintenance and Follow-Up
See the patient at one week, then monthly for three months, then every three to six months after healing. Inspect tissue, torque, hygiene, and occlusion at each visit. Photograph and record small changes before they become big ones.
Teach effective home care for full-arch bridges. Interdental brushes, water irrigation, and specific flossing aids matter. Ask about smoking at every visit, because it still matters.
Selecting a Zygomatic Implant Specialist
Choose an oral and maxillofacial surgeon or implant specialist with significant zygoma experience. Ask for documented cases and long-term follow-up. Prosthetic-led planning should be the rule, not the exception.
An in-house digital lab with CAD and CAM improves accuracy and turnaround. A coordinated team keeps surgery, provisionalization, and occlusion aligned. Skilled people, clear plans, better outcomes.
Takeaway
For patients with “no bone” diagnoses, zygomatic implants can deliver stable, same-day teeth with fewer stages and shorter timelines. At Surya Dental Care, Trichy, we plan prosthetics first, confirm anatomy with CBCT, and select anesthesia that fits the case, IV sedation or local with premedication. You’ll get an itemized plan, clear maintenance steps, and realistic timelines. If you’ve been told implants aren’t possible, get a second look. Book a consultation with Surya Dental Care and see if zygomatic implants fit your case.